Report: Trends in Nursing 2024

This past year posed unique challenges for nursing worldwide, from heightened workloads to ongoing strikes. At IntelyCare, we have a direct line to healthcare professionals, so we took the initiative to make their voices heard. To gather valuable insights into the key trends in nursing, we conducted a survey with nurses and nursing assistants and received more than 5,000 responses.
It may come as no surprise to learn that a whopping 83% expressed worry over the state of the profession. Our analysis offers a glimpse into nursing professionals’ experiences, perspectives, and concerns — a snapshot of what it means to be on the job today. The major trends we uncovered include:
- Job turnover: 76.9% of nursing professionals plan to seek a new nursing job in 2024.
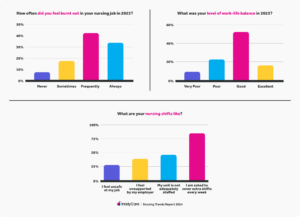
- Burnout: 75.8% experienced burnout in 2023. Only 6.9% reported never feeling burned out.
- Career dissatisfaction: 54.9% plan to stay in nursing, but 45.1% are considering leaving the profession altogether in 2024.
- Staffing concerns: 46.4% express worry regarding staffing issues, and better staffing surpassed even a higher salary as the one thing that would have the most positive impact on their jobs.
- Patient ratios: 76.3% of CNAs, 92.3% of LPNs, and 62.9% of RNs said that they were responsible for 9 or more patients on a regular shift in 2023.
- Lack of support: 39% didn’t feel supported by employers.
“Bring back humanity. Rushed care is equivalent to no care.” — Survey respondent
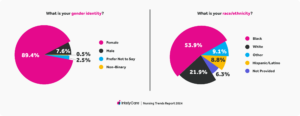
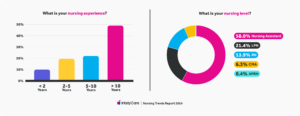
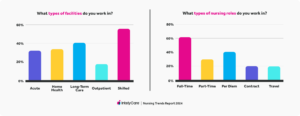
2024 Survey: Demographics of Respondents
Realities of Nursing Today: Trends and Perspectives
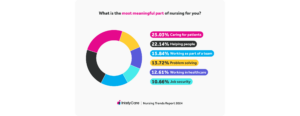
Nursing is hard work, but it offers undeniably unique rewards. Respondents chose “helping people” and “caring for patients” as the top two most meaningful parts of the job.
But what’s the actual experience like? Do the rewards outweigh the challenges?
Nearly 76% of nursing professionals reported burnout, yet only 31.8% felt they had inadequate work-life balance. How is that possible?
The Challenges Nursing Professionals Face
The vast majority of nursing professionals (75.8%) who replied to our survey said they experienced burnout in 2023. Things that contribute to burnout include:
- 84% were often asked to cover extra shifts — this includes 50.9% of respondents who were asked multiple times a week and 19.2% who were asked daily.
- 46.4% believe that their unit was understaffed.
- 39% felt unsupported by their employer.
- 31.8% struggled with work-life balance.
- 28% felt unsafe at their job.
Notice that nearly 76% of nursing professionals reported burnout, yet only 31.8% felt they had inadequate work-life balance. How is that possible?
The term “burnout” is often used to describe emotional exhaustion, lack of motivation, and feelings of frustration due to tough work conditions. In other words, burnout measures the intensity of nursing professionals’ work hours.
Work-life balance is focused on time distribution — how much time nursing professionals spend at work versus at home. Even though many nursing professionals work traditional 12-hour shifts three days a week, the intensity of the work can still outweigh the time off. A more balanced schedule can reduce stress, but days off won’t make up for the fact that time spent at work is emotionally and physically draining. That may give insight into why 76% of our respondents reported burnout while 68.2% shared that they enjoy a work-life balance.
So what else could be contributing to the demands of the job? A combination of baby boomers reaching retirement age and the prevalence of chronic health conditions among that generation (such as heart disease, diabetes, and respiratory disorders) means more and more nursing professionals are and will continue to be needed to take care of these patients. Exacerbating this issue are the facts that fewer people are entering the nursing profession and more RNs than ever are leaving nursing. This will only add to the challenges nursing professionals face on the job.
Current Trends: What Matters to Nursing Professionals Now?
To gain a thorough insight into the anticipated trends for the coming year, we asked: What do you believe will be the most significant trend in nursing for 2024? Respondents selected all that applied:
- Pay: 51.1%
- Time with patients: 33.9%
- More nursing professionals leaving the profession: 31.4%
- Voice in management decisions: 22.2%
- Workplace danger: 16.3%
- Time spent on documentation: 16.2%
- Increase in AI or new tech: 13.9%
Future Trends: What Do Nursing Professionals Want in 2024?
Nurses and nursing assistants have their own work preferences, but what might improve their jobs the most? We presented five options in our survey: more money, better staffing ratios, better work-life balance, increased safety, and more decision-making power.
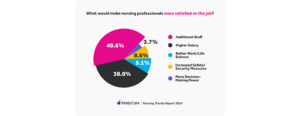
The top two picks were additional staffing, followed closely by better pay. Those two elements are of such critical concern to nursing professionals that the other options were dwarfed in comparison.
Staffing ratios directly affect the level of patient care, which is what nursing professionals are all about, but 41.4% of them felt they weren’t able to spend quality time with their patients in 2023. Take a look at what some respondents told us:
- “I wish I had more time to meet my patients’ wants and needs related to their care. Due to the nurse-to-patient ratio, I am always behind and struggling to catch up.”
- “I love my job, I’d just like a little more pay and fewer patients so I can really care for them.”
- “More time caring for the patient, less caring for the chart.”
- “Bring back humanity. Rushed care is equivalent to no care.”
Based on the overall rankings, let’s take a closer look at what matters the most to these workers.
1. Additional Staffing Is the Top Priority for 40.6% of Nursing Professionals
Nurses and nursing assistants often find themselves handling a multitude of tasks and responsibilities. Adequate staffing not only helps in distributing the workload more evenly but also ensures that they can provide quality care to patients without feeling overwhelmed, which can contribute to an onset of burnout.
And when you think about the leading reasons nursing professionals love their jobs — helping people and caring for patients — this makes sense. Nursing professionals want to be able to do their jobs well. They want to give the type of care they know they’re capable of providing, and they can’t do that when their facilities are understaffed.
From the Trends in Nursing survey:
“Nursing is extremely hard work — demanding, with high burnout rates. All facilities, including acute care, LTAC, LTC, and day programs, NEED to staff better so people can be taken care of.”
2. 38% of Nursing Professionals Prioritize a Higher Salary
In a world where inflation impacts the purchasing power of income, a salary that keeps pace with economic changes becomes vital in retaining nursing professionals. A competitive and fair salary not only recognizes the value of their education, training, and daily responsibilities but also helps alleviate the very real financial pressures they may encounter — everything from tuition and childcare payments to grocery and gas bills.
From the Trends in Nursing survey:
“Pay has decreased and continues to lag.”
3. 9.1% of Nursing Professionals Would Choose a Better Work-Life Balance
Nursing is a demanding profession, and offering flexibility allows nurses and nursing assistants to juggle their work and personal commitments more effectively. With the ability to tailor their schedules, nursing professionals can achieve a healthier equilibrium, reducing stress and preventing burnout.
From the Trends in Nursing survey:
“Have a[n employer] that takes care of their employees.”
4. Increased Safety Is the Top Concern for 8.6% of Nursing Professionals
Incidents of workplace violence against nurses are on the rise, prompting calls for the government to step in and take protective action. In addition to having adequate staffing, employers would want to consider offering measures like de-escalation training and increasing security to help ensure both physical safety and quality patient care. Cultivating a bullying-free culture is equally crucial for fostering emotional safety.
From the Trends in Nursing survey:
“We want to be safe! We want our patients to be safe!”
5. Just 3.7% of Nursing Professionals Prioritize More Decision-Making Power
Empowering nurses and nursing assistants to make important decisions regarding patient care and workflow has been shown to enhance job satisfaction. When they have a say in the decision-making process, nursing professionals feel a greater sense of engagement in their work. This autonomy can help foster a deeper commitment to the profession.
From the Trends in Nursing survey:
“Make nurses feel like they are appreciated.”
“The results of the 2024 survey showed us that the nurses and aides we’ve kept in the workforce are not in it for the money. So much has been made about nursing wages in the last few years, and rightfully so. But if we’ve learned anything it’s that throwing money at the staffing problem isn’t only unsustainable, it doesn’t work. As employers, it’s time to meet nurses where they’re at and rethink how we manage our workforces and investments to meet their needs. You need to look at things like flexibility and understand what that truly means to individuals in your workforce. You need to look at shift diversity and understand that if you’re not offering roles beyond full-time, you’re limiting your recruiting pool. And lastly, plan ahead. There are cyclical events that impact the ability to stay properly staffed and must be accounted for.”
— Sean Carney, Vice President of Client Services, IntelyCare
Why Better Staffing Is a Key Concern
Now, let’s address the elephant in the room — the continuing effects of understaffing in the nursing profession. Our survey found that nearly 51% of respondents were asked to cover an additional shift more than once per week.
Without enough healthcare workers to support a facility, the quality of care that’s able to be provided to patients can be compromised. Furthermore, being a nursing professional can become difficult and at times dangerous on a number of levels: physical, emotional, and legal.
1. Physical Safety
Nursing professionals face physical safety challenges, with 16.3% identifying workplace danger as a key issue in nursing and 28% expressing safety concerns. Adequate staffing is essential, particularly for tasks like patient transfers and managing agitated individuals. Workplaces, especially in psychiatric settings, need secure layouts. This includes thoughtful building designs and securing the nursing station. Additionally, personal safety requires that essential supplies — like gloves and masks — must be readily available.
From the Trends in Nursing survey:
“It is dangerous being a nurse without LTC ratios.”
2. Emotional Safety
Nurses and nursing assistants face real psychological challenges — burnout, stress, PTSD, and even suicide risk.
Nursing professionals must sometimes work beyond their stated hours to cope with the demands of the job and may still face criticism from patients and supervisors. And yet, nursing professionals will overextend themselves. This habit can lead to moral distress — a condition that happens when institutional constraints prohibit these healthcare workers from doing their jobs correctly and to the best of their ability. To address this dilemma, nursing professionals need more than just a wellness app — they need real support.
From the Trends in Nursing survey:
“Burned out. Expectations exceed human limits, dictated by insurance and state regulations that never engage directly with the patients.”
3. Legal Safety
Legal concerns can weigh heavily on nursing professionals, especially in understaffed units where incidents are more likely to occur. Nursing professionals can ask their facility what steps it takes to ensure compliance with the state’s staffing mandates (if there are any) and how it protects its employees, knowing they could be subject to legal ramifications if an incident occurs and a patient is injured or dies.
States have different laws regarding mandatory overtime, and in some states, a nursing professional can be fired for refusing to work beyond their agreed-upon hours — even when they are experiencing moral distress and don’t feel it’s safe for them or their patients to accept overtime. In such instances, a nursing professional can also request a Protest of Assignment form (also known as Assignment Despite Objection), which could help to provide them with some legal protections should an adverse event occur while they’re on an assignment under protest.
From the Trends in Nursing survey:
“[Employers need to be] protecting employees more from situations that arise at the facilities.”
“We all know what the proper ratios for safe staffing are in our various settings. The fact that so many clinicians are caring for well over these recommended limits is very detrimental to patients. These are nurses and aides who entered the profession to impact patient care but now find themselves enduring longer work hours and heavier workloads. The guilt that comes with not giving patients the time and attention they deserve takes a real emotional toll on nurses. And when you have a workforce that is motivated to provide quality care, you can’t expect to retain them if you’re hindering that.”
— Lynn Barry, Vice President of Clinical Operations, IntelyCare
Key Takeaways From Trends in Nursing
If you’re a nursing professional who questions your career choice, this survey lets you know that you’re not alone. Furthermore, this workforce is nothing if not determined: Nearly 74% of our respondents believe that they will spend more time talking with patients in 2024, despite the challenges they face, even if that means they’ll need to find a new job in order to make that human connection happen.
But for the nursing profession to be the rewarding and fulfilling career it’s meant to be, policies must change and healthcare employers will need to provide their support. Read our employer-facing analysis for more insight into what facilities can do to positively impact the nursing profession.
Methodology
In December 2023, IntelyCare surveyed nursing professionals across the United States to gain a better understanding of their attitudes toward the profession. We received completed surveys from 2,977 respondents and partial surveys from 2,035 respondents. The survey included 26 questions aimed at understanding nursing job trends in 2024, what leads to a meaningful nursing job experience and what challenges it, why nursing professionals leave or accept new jobs, and more.
Survey respondents spanned across multiple provider types, including Nursing Assistants (58%), Licensed Practical Nurses (21.4%), Registered Nurses (13.9%), Certified Medical Assistants (6.3%), and Advanced Practice Registered Nurses (0.4%), and almost half of respondents (49.1%) had over 10 years of nursing experience. The respondents also worked in a variety of care settings, including skilled nursing (55.6%), long-term care (40.4%), home health (33.6%), acute care (31.9%), and outpatient care (17.5%).
All participants responded anonymously and the data was validated and analyzed by the IntelyCare Data Science Department. For all inquiries regarding the report, please contact marketing@intelycare.com.
Legal Disclaimer: This article contains general legal information, but it is not intended to constitute professional legal advice for any particular situation and should not be relied on as professional legal advice. Any references to the law may not be current as laws regularly change through updates in legislation, regulation, and case law at the federal and state level. Nothing in this article should be interpreted as creating an attorney-client relationship. If you have legal questions, you should seek the advice of an attorney licensed to practice in your jurisdiction.